Cataracts
Emulating the young human eye, which sees clearly in the distance and at close range, remains the ultimate goal following cataract surgery.
Dr Holcombe is a highly skilled eye surgeon and uses the advanced keratometry of the Lenstar optical biometer and premium intraocular lens implants to bring you as close as we can to that goal.
What is a cataract?
Inside our eye is a structure called the lens. This helps focus light onto the back of our eye (retina) to facilitate vision. A cataract refers to the clouding of the lens itself. Some people think that there is a film that grows over the eye, but it is actually a clouding of the whole lens structure. Most cataracts are caused by the normal ageing process. This means that if you live long enough, you will develop cataracts. In some people cataracts develop at a younger age. Factors that may cause the early development of cataracts include eye trauma, ultraviolet light exposure, smoking, some medications, and diseases such as diabetes.
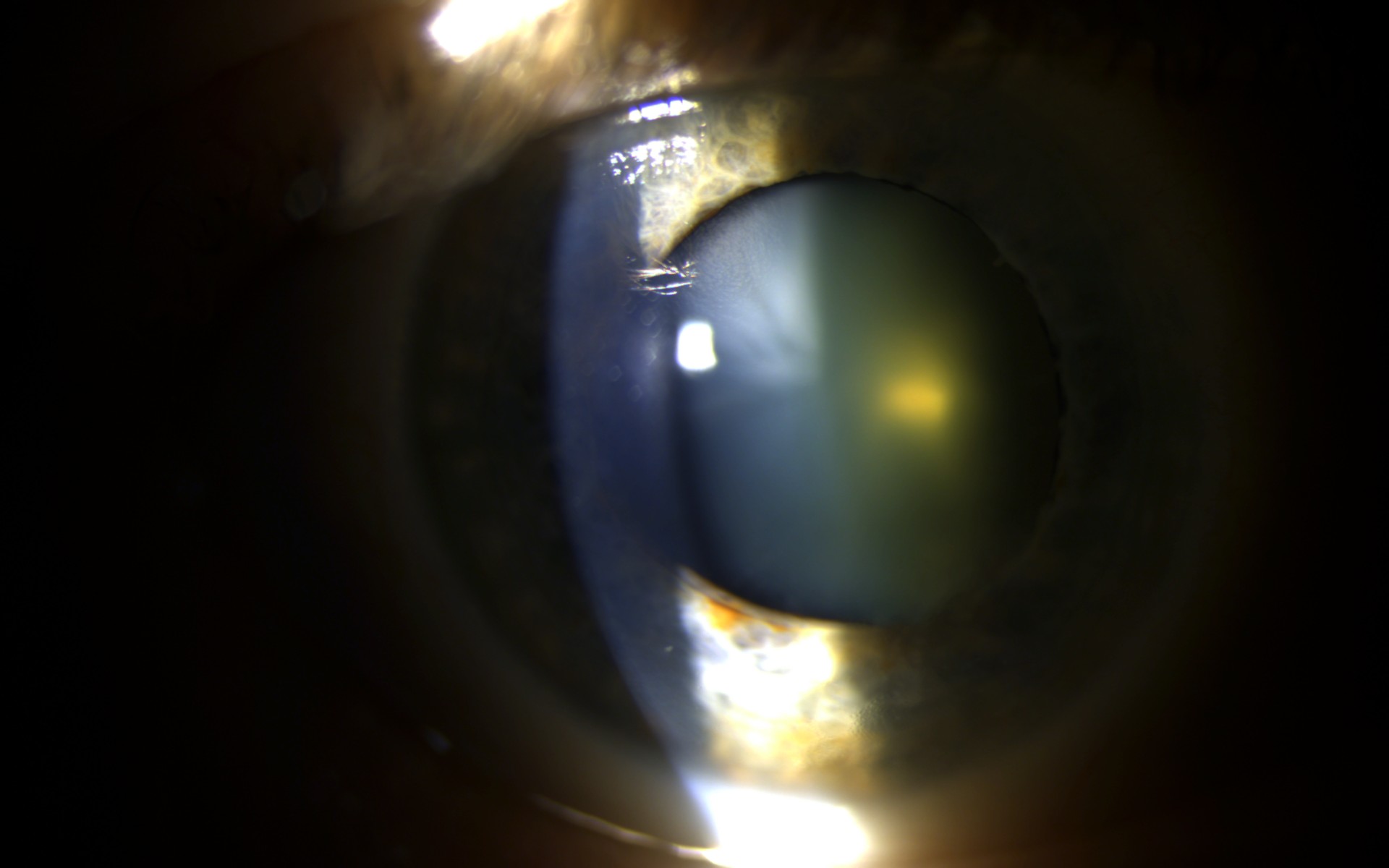
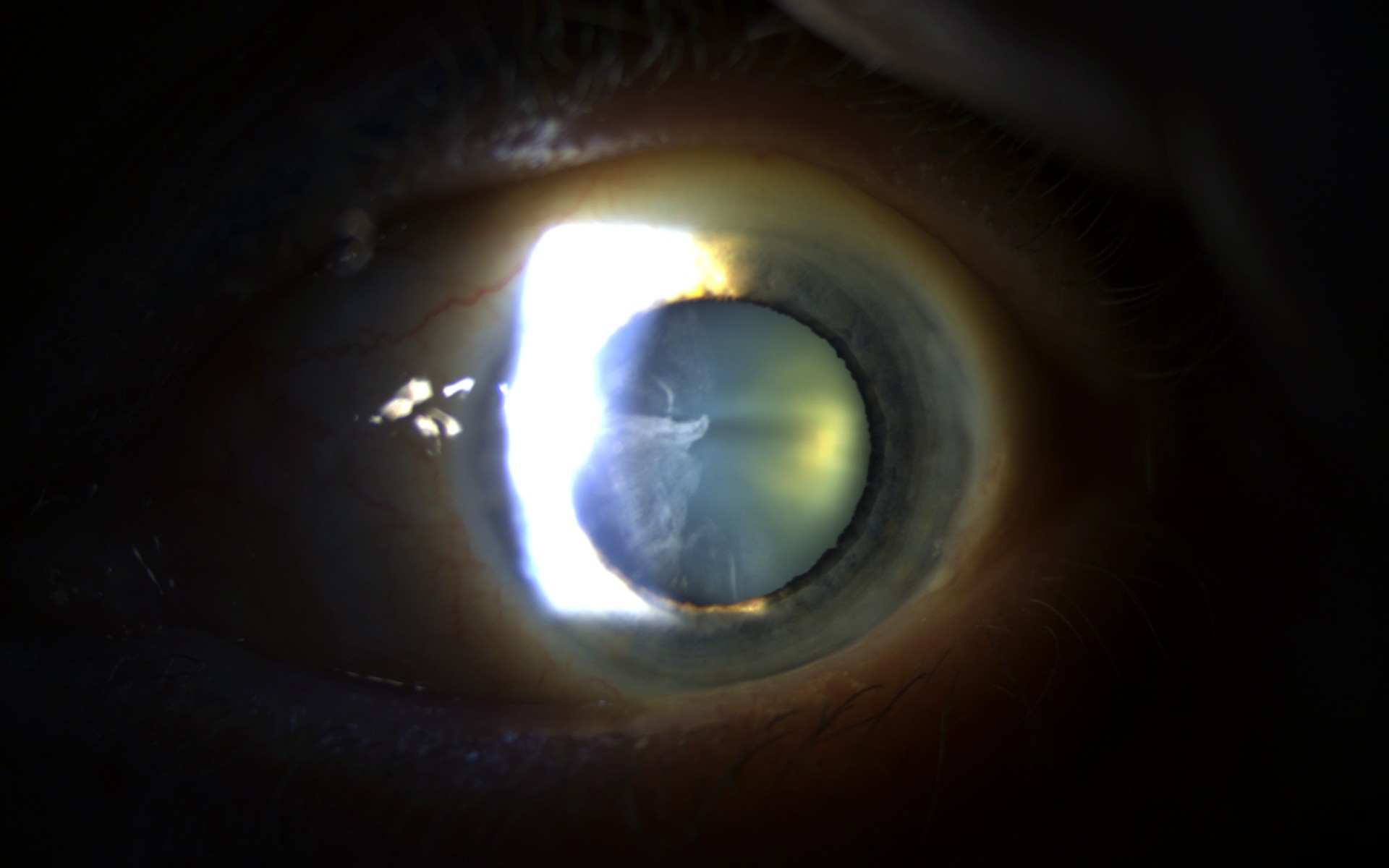
Specialist slit lamp examination reveals the clouding of the lens which is the key feature of cataracts
From the day you are born to the day you take your last breath, the lens inside the eye becomes increasingly yellow tinted. This constitutes a cataract, but at the early stages it may not affect your vision at all. As the cataracts progress however, you may notice any or all of the following:
- you have difficulty with fine detail work, such as threading a needle or reading small print
- you need to update your glasses or contact lenses more often and they just don’t seem to give you the clarity of vision you are used to
- you are bothered by symptoms of glare; this is noticed particularly when driving at night and oncoming car headlights are dazzling, or other lights are “fuzzy” or have a “halo” or “glow” around them
Cataract surgery
Currently the only treatment for cataract is surgery. Many people ask, when is the right time to do surgery? The answer with any surgical procedure is a balance of the risks and benefits, but surgery should be considered once your cataracts are interfering with your life, and are preventing you from doing the things that give you enjoyment. Occasionally some people are not bothered by their cataracts, but their vision has worsened to the point that they no longer meet the legal standard required for driving vision. In this situation if the patient wishes to continue to drive, then surgery would be required.
Cataract surgery is the most common eye operation, but it is not a trivial procedure. It is a delicate operation in which the cataract needs to be removed, whilst preserving certain structures within the eye in order to be able to place a new lens implant into the eye at the end of the operation. As the natural lens of the eye is an optical structure, an optical structure needs to be replaced in order to refocus the eye at the end of the procedure. More will be discussed on this later.
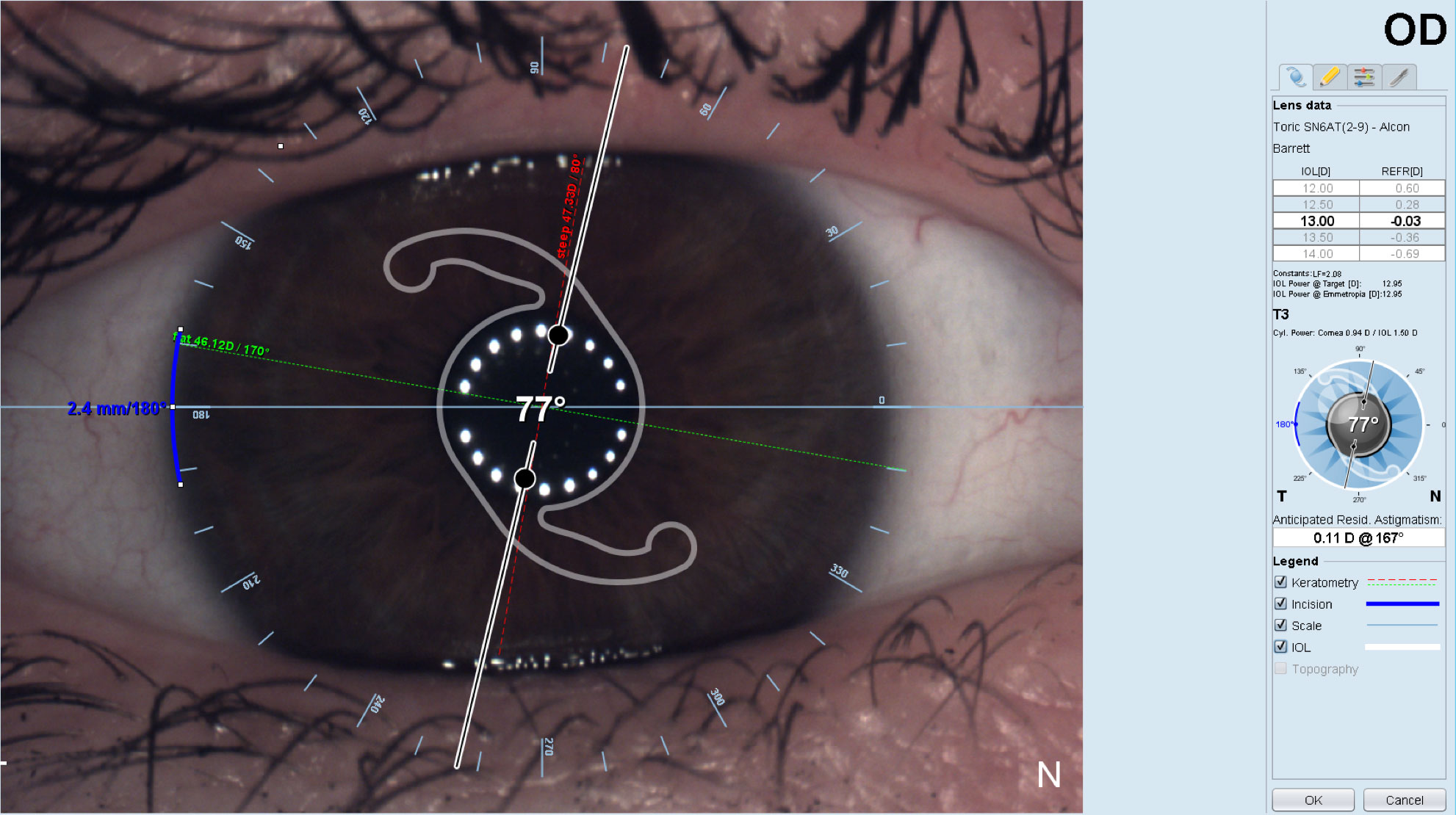
Cataract surgery planning
Cataract surgery is usually a day procedure performed under a local anaesthetic with twilight sedation. Dr Holcombe uses topical anaesthetic drops and gentle sedation to facilitate your surgery thus avoiding the risks associated with eye blocks. Once the local anaesthetic and twilight anaesthetic is administered, the operation is performed. A small 2.2 mm incision is placed on the eye and the cataract is broken up inside the eye into tiny pieces and “vacuumed” out. The whole procedure is generally painless. Once the cataract is removed an intraocular lens implant is inserted into the eye.
Prior to your operation you will have your eye measured on the Lenstar LS900. This advanced machine is the first of its type in Toowoomba.
Lenstar optical biometry with advanced keratometry is used to precisely plan individualised cataract surgery
After your surgery you will spend a short time in recovery then you will be ready to leave. You will need someone to drive you home. There is minimal discomfort from cataract surgery performed with local anaesthetic and twilight sedation. Some patients say they have no discomfort, some say that the eye feels a little scratchy. Over the counter medication such as paracetamol, if anything, is usually all that is required to control any discomfort. An information sheet and eyedrops will be provided after surgery and a post-operative appointment will be made for you.
Intraocular lens selection
The original goal of cataract surgery was to clear the line of sight, and glasses were used to fine tune the focussing to provide the patient with sharp vision. With the accuracy of the measurements provided by the Lenstar LS 900, new calculation methods for manipulating this data, and the accuracy of implantable lens manufacture, we now live in an era where it is possible to ‘reset’ the focus of the eye at the time of cataract surgery. Whilst the results anywhere in the world are still not 100% accurate, with advances in technology they are better than they ever have been before. Hopefully by the time I need my cataracts done the calculation accuracy will reach 100%!
How I reset your eye’s focus at the time of cataract surgery really depends on what you like to do with your vision, the activities you participate in, and the lifestyle that you lead. The ‘holy grail’ of intraocular lens implantation is to be glasses free for everything – that is, see in the distance and read small print up close without the aid of glasses, much like many young people do.
Unfortunately the technology does not exist yet whereby this outcome can be provided reliably and without side effects to patients. Once again, something that I hope will be sorted by the time I need my cataracts done! Consequently, compromises and decisions must be made about the type of vision, and hence lens implants you would like.
Essentially there are four main choices:
Your vision options
If you are considering cataract surgery, Dr Holcombe can discuss all your available options to find a strategy that will most closely match the visual requirements of your lifestyle.
All surgical procedures carry some risk. The information provided here is for general educational purposes only. Please contact Dr David Holcombe of Toowoomba Ophthalmic Consultants to discuss the options that are appropriate for your individual situation.
FAX (07) 4670 9677
Monday - Thursdays 8:30 am - 4 pm